NEW! People You Should Know Podcast: had the wonderful opportunity to share my story for a new podcast. Click here to take a listen Megan King- Ehlers-Danlos Syndrome Make sure you listen to the other podcasts that are featured. There are so many amazing individuals with amazing stories that you'll most definitely want to take a listen to.
One of the hardest things after any surgery is getting up out of bed and walking the halls. For me, there is a constant internal battle because half of my mind is saying, "I don't want to get up and walk because it hurts, and I'm tired," while the other half of my brain is trying to motivate myself by saying, "Get up and walk so you can get strong enough to go home." With Ehlers-Danlos Syndrome the more you don't move, the weaker all of your joints will get because your muscles will weaken. In EDS, strong muscles are key to keeping joints more stable.
 |
| To walk or not to walk??? |
 |
| View from my new room of the Museum of Science & Industry. I would much rather be strong enough to be outside, versus being in the hospital. |
It was a more "exciting" day because my sister stopped by to visit me. I was so happy to see her because she was able to get my hair up for me since I can't reach the top, or behind my head. My hair had been driving me nuts because it was getting caught in my halo. Fortunately she solved the problem. One might not realize how ridiculously hard it is to get your hair brushed while in the halo. It's even more difficult to get it into a ponytail because you have to slide the front hair under the bar that goes over the top of your head in addition to behind/above the screws over your ears. It involves much more than you'd ever realize. It's really time consuming initially because you're learning how to even do the task. My sister was officially dubbed the, "Halo Hairstylist". A few days before I had my halo application I went and had my hair cut shorter because I thought it would be easier in the halo. For me, I think having my hair shorter made it harder to get it up in a ponytail.
 |
| I have absolutely no idea what we were doing except being weird and she got me to smile. |
 |
| A+ for her getting my hair up and off of my face and neck! |
 |
| Once my hair was up, I learned my incision was longer than I initially had anticipated. When my hair was down in the previous post, I didn't realize how high the incision went. Surprise! |
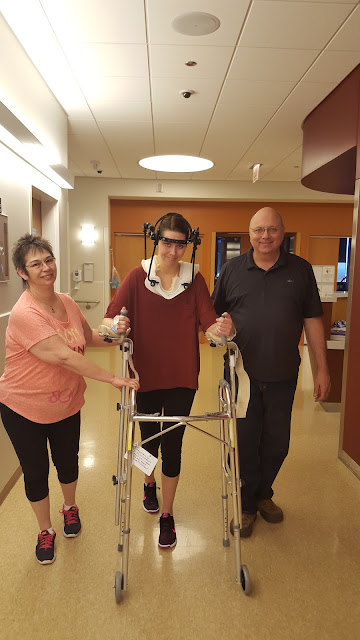 |
| A quick "smile at the camera" as my parents and I were trying to walk all the way around the nurses station. You can tell just how thrilled my parents and I were. |
April 17, 2016 Post-Op Day 5:
I was on a mission this day. What's the mission you might ask? To get my left my arm in a sling because I was officially fed up that I was in a hospital, and nobody had any idea of what to do to immobilize it. The pain over my left scapula was increasing, and it was making me more cranky than I already was. Between the neck pain, and the scapula pain I wasn't the most pleasant individual to be around; however, with every other obstacle that has ever been put in my path, I think, and figure out a solution to get around it. This was no different, and this is how it all played out. The nurse, as well as the physical and occupational therapists had left my room officially saying there wasn't anything they could do. I could understand the nurse not having too many ideas since it's not their area of training, but I was not pleased at all with the physical or occupational therapists. If they weren't going to think of a solution then I guess I would have to figure it out myself.
My mom and sister were with me. I remember standing up, and saying, "That's it! We're going to be 'old time mountain women' and go back to the old days and make a sling". I had my mom, and sister take the sheet off of my bed because that's what we were going to use to make a sling to immobilize my arm. I knew we could make something that would go around my torso that would not put any pressure on the halo, and it would not put any pressure on my neck. It honestly took maybe 5 minutes to make a sling. The problem was solved. It wasn't rocket science. This was the final product and it worked like a charm!
 |
| Walking unassisted! You should have seen the look on the nurses faces when they saw me out of my room without a walker, and with my arm in a sling made from a bed sheet. It was priceless! |
 |
| Very fitting words that were right outside my hospital room. I did one lap around the nurses station and noticed these words when I got back to my room. "Put one foot in front of the other!" |
 |
| When you're post-op, one lap around the nurses station is exhausting. |
April 18, 2016 Post-Op Day 6 aka Discharged Home Day!
You may or may not notice I am in the exact same clothes that I was in the day before. I am one of those people who notices details. After surgery it takes a lot of energy to get changed, and do simple tasks. If it's not necessary to use that "energy storage" then don't. Save your energy to do something more productive, like walk. Also, in my situation, if I were to change, that would mean I would have to take off the "sheet sling". My arm was in a relatively comfortable position. When you find those comfortable positions, you don't mess around. You take advantage of them for as long as you possibly can!
The day before, I told my parents, and Dr. F I wanted to go home the following day (April 18th). I was so tired because nurses are always coming in at all hours of the day, and night to check vitals, and I was hurting. My shoulder/scapular surgeries were postponed due to the severity of my neck, and I knew I would be more comfortable at home. At this point I was on all oral medications so there really wasn't a need to be in the hospital. Dr. F told me there was absolutely no rush, and I was allowed to stay longer if I wanted to. I wanted my recliner, and I wanted my dog Daisy. She helps keep me calm, and petting her is soothing; essentially, it's pet therapy.
My parents and I were hoping that I would be discharged in the morning since we were in Chicago, and we wanted to avoid rush hour traffic. It wasn't the end of the world, but I didn't get discharged until around 5:30-6:00 p.m. To those that aren't familiar with Chicago, that is rush hour hell with bumper to bumper traffic. Since we were at the hospital pretty much all day, it turned into a busy one.
Before being discharged, I had to pass the protocol from the physical therapists perspective. She came by in the afternoon. This was a new physical therapist and she was a hoot. She came by to make sure I could walk okay, and had me do stairs because we have stairs in our house. She was very nice. I liked her a lot. I passed my walking, and stairs test with flying colors. She was impressed that I was able to walk so easily with the halo. She told me most people are pretty wobbly, and have trouble finding their center of balance. I told her I've had a lot of surgery, and I've been in a lot of various braces that have had me lopsided. Being lopsided forced me to get good balance; in that respect, all those previous surgeries prepared me for the halo. I didn't have a hard time learning how to walk or do stairs at all. To anyone that may be having to face neck surgery, I would suggest getting your body in as best of shape possible. When you go into surgery strong, you typically have an easier recovery; that doesn't mean it won't be hard.
 |
| She was funny; she couldn't get over my height |
 |
| Going up the stairs |
 |
| Coming down the stairs |
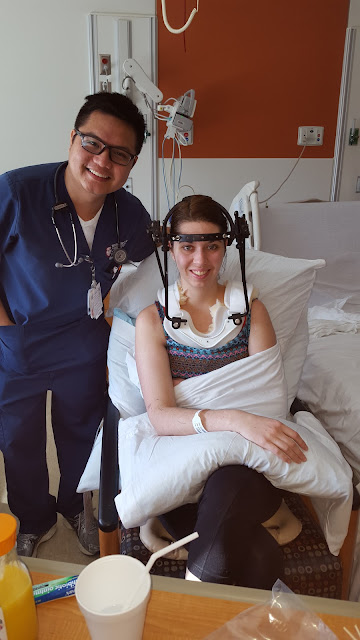 |
| My nurse and I. |
Later in the day, Dr. F stopped by with one of his associates. Once again, he told me that I could stay longer, and that he liked coming to visit me. I chuckled but told Dr. F I would be more comfortable at home, and would be seeing him soon for post-op visits. While in my room he decided to take off the dressing that was applied over my incision. It was at this time when I got a better idea of what my incision looked like. Those white pieces you see that look like tape are called steri-strips. They help the incision heal, and will fall off on their own.
Final Question: Can I please take a picture with you because I get my picture taken with every doctor that has helped me? I think he was little shocked by this question but said, "Yes, here you can sit next to me on the couch." My mom went to take our picture but with the sun at our backs, you couldn't see our faces. So we had to stand instead, and he said, you're going to be taller than me if we stand. I told him I'll slouch down a little then.
 |
| Dr. F & I |
 |
| Thumbs up! Home at last! |
 |
| https://www.pinterest.com/pin/37225134393324190/ |
Next post will be about some humorous hurdles and obstacles that I had to overcome now that I was home.
If there is anybody that has Ehlers-Danlos Syndrome (EDS), is in/was in a halo that would like to connect, please feel free to email me at kingmeg19@gmail.com
* *If you have a Facebook account, click here and "LIKE" my page: Meg's EDS Medical Journey
** Follow me on Instagram: https://www.instagram.com/thetravelinghaloofhope/








































